Beyond the Hospital Walls: The Economics of Shifting Care Sites
Analysis of shifting care sites in response to economic pressures, focusing on Hospital-at-Home trends in Psychiatry and Pediatrics.

Key Developments
The US healthcare sector faces significant economic strain, with national expenditures projected to outpace GDP growth significantly over the next five years. By 2033, healthcare spending could reach 20.3 percent of GDP. Simultaneously, the population aged 65 and older is growing at nearly 3 percent annually, driving higher acuity and demand for chronic care.
The “Reimagining sustainable healthcare and business models” from McKinsey provides a detailed evaluation of the issue: https://www.mckinsey.com/industries/healthcare/our-insights/reimagining-sustainable-healthcare-and-business-models#/
As they wrote, in response to the challenges, the industry is pivoting toward four key archetypes, with “shifting sites of care” emerging as a primary lever. A clear example of this evolution is Total Joint Replacement (TJR). Between 2018 and 2023, inpatient TJR procedures plummeted from 78 percent to just 9 percent, shifting largely to outpatient and ambulatory settings. This transition reduced the overall cost per episode by 9 percent while maintaining or improving complication rates.
Having led Sustainable Development and Innovation at Boehringer Ingelheim in the CEE region for several years, this report naturally caught my attention.
I want to dig deeper into specifically the Hospital-at-Home (HaH) topic.
Why This Matters
While surgical shifts like TJR are well-established, the “Hospital-at-Home” (HaH) model represents a critical evolution for acute medical care. Distinct from standard home health, HaH substitutes acute inpatient care for patients who are stable enough for remote monitoring but sufficiently ill to otherwise require a hospital bed.
The model relies on command centers and wearable technology to facilitate 24/7 monitoring. This approach addresses capacity issues—reducing “bed blocking” for high-acuity cases—and mitigates hospital-associated deconditioning, particularly in the elderly. The economic logic parallels the surgical shift: utilizing lower-cost sites for high-quality care delivery.
The Broader Context
What is Hospital-at-Home? HaH is a healthcare delivery model that provides acute, hospital-level care in a patient’s home. It is crucial to distinguish this from standard “home health care.”
Home Health Care is typically for low-risk recovery or chronic management.
HaH is a substitution model: these patients are sick enough to require a hospital bed right now (e.g., severe pneumonia, heart failure) but are stable enough to be monitored remotely.
Think of it as admitting the patient to their own bedroom rather than a ward.
How it Works
The workflow relies on confirming the patient has a safe home environment, followed by setting up a domestic “command center” with internet-connected tablets and wearable patches for 24/7 monitoring.
Daily Care: Nurses visit 1–2 times daily for tasks like IVs or blood draws, while doctors conduct virtual rounds.
The Benefit: It reduces “bed blocking” in physical hospitals, lowers costs, and significantly helps elderly patients avoid hospital-associated delirium and infections.
The Challenge: Success depends on bridging the “tech divide” for older patients and managing logistics (like delivering portable X-rays to the suburbs). It also places a higher burden on family caregivers compared to a fully staffed ward.
My Research Approach
To understand the current landscape, I turned to PubMed. A search for “hospital at home” yielded over 10,000 results in the last year alone.
I analyzed these 10,000 citations—focusing on titles, abstracts, keywords, and MeSH terms—and utilized ChatGPT to classify the data to see where the concept is gaining the most traction.
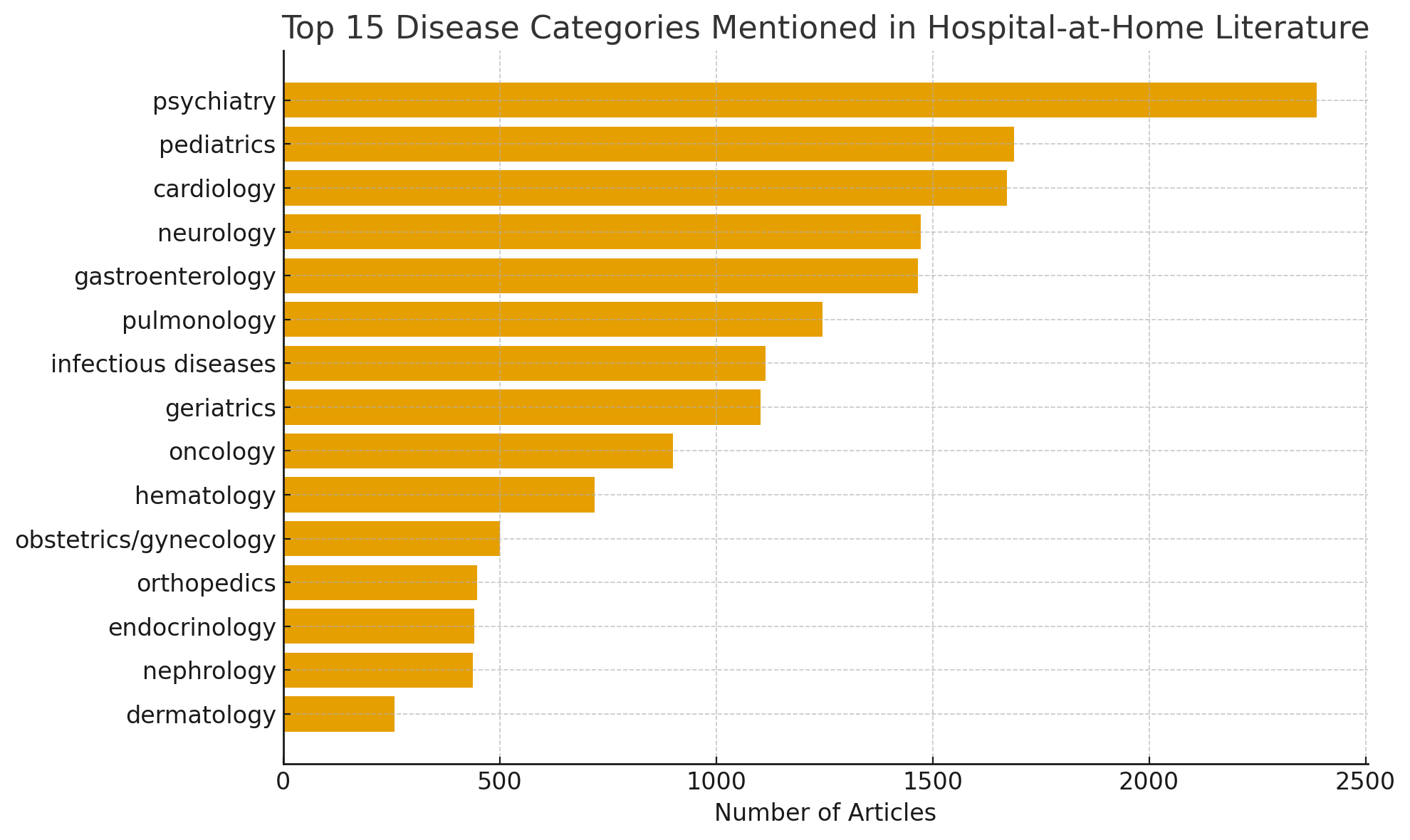
A text mining analysis of over 10,000 recent PubMed articles reveals distinct trends in HaH adoption. Contrary to the assumption that geriatric or internal medicine dominates the literature, Psychiatry ranks first with 2,387 articles, followed surprisingly by Pediatrics (1,689) and Cardiology (1,672).
| Rank | Disease Category | Number of Articles |
|---|---|---|
| 1 | Psychiatry | 2,387 |
| 2 | Pediatrics | 1,689 |
| 3 | Cardiology | 1,672 |
| 4 | Neurology | 1,473 |
| 5 | Gastroenterology | 1,466 |
| 6 | Pulmonology | 1,246 |
| 7 | Infectious Diseases | 1,114 |
| 8 | Geriatrics | 1,102 |
| 9 | Oncology | 900 |
| 10 | Hematology | 719 |
| 11 | Obstetrics / Gynecology | 501 |
| 12 | Orthopedics | 448 |
| 13 | Endocrinology | 441 |
| 14 | Nephrology | 438 |
| 15 | Dermatology | 258 |
The prominence of Pediatrics suggests a strong clinical drive to minimize the stress of hospitalization for children. However, widespread adoption faces distinct hurdles, including the “tech divide” among patients and the logistical complexity of delivering hospital-grade interventions—such as IVs and X-rays—to residential addresses.
Looking Ahead
Shifting care sites offers a validated mechanism to manage costs and improve outcomes. Moving forward, scalability will depend on aligning financing mechanisms and addressing the operational barriers—specifically caregiver burden and logistical density—that currently constrain these models beyond pilot programs.